Abstract
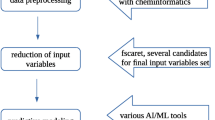
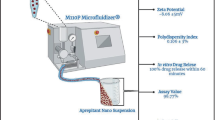
In the present study, liquisolid formulations were developed for improving dissolution profile of aprepitant (APT) in a solid dosage form. Experimental studies were complemented with artificial neural networks and genetic programming. Specifically, the type and concentration of liquid vehicle was evaluated through saturation-solubility studies, while the effect of the amount of viscosity increasing agent (HPMC), the type of wetting (Soluplus® vs. PVP) and solubilizing (Poloxamer®407 vs. Kolliphor®ELP) agents, and the ratio of solid coating (microcrystalline cellulose) to carrier (colloidal silicon dioxide) were evaluated based on in vitro drug release studies. The optimum liquisolid formulation exhibited improved dissolution characteristics compared to the marketed product Emend®. X-ray diffraction (XRD), scanning electron microscopy (SEM) and a novel method combining particle size analysis by dynamic light scattering (DLS) and HPLC, revealed that the increase in dissolution rate of APT in the optimum liquisolid formulation was due to the formation of stable APT nanocrystals. Differential scanning calorimetry (DSC) and attenuated total reflection FTIR spectroscopy (ATR-FTIR) revealed the presence of intermolecular interactions between APT and liquisolid formulation excipients. Multilinear regression analysis (MLR), artificial neural networks (ANNs), and genetic programming (GP) were used to correlate several formulation variables with dissolution profile parameters (Y 15min and Y 30min) using a full factorial experimental design. Results showed increased correlation efficacy for ANNs and GP (RMSE of 0.151 and 0.273, respectively) compared to MLR (RMSE = 0.413).









Similar content being viewed by others
References
Poli-Bigelli S, Rodrigues-Pereira J, Carides AD, Julie-Ma G, Eldridge K, Hipple A, et al. Addition of the neurokinin 1 receptor antagonist aprepitant to standard antiemetic therapy improves control of chemotherapy-induced nausea and vomiting. Results from a randomized, double-blind, placebo-controlled trial in Latin America. Cancer. 2003;97:3090–8.
European Marketing Authorization, Emend (Aprepitant): Summary of Product Characteristics. 2003. Available at: https://www.medicines.org.uk/emc/medicine/13868. Accessed 18 June 2017.
Wu Y, Loper A, Landis E, Hettrick L, Novak L, Lynn K, et al. The role of biopharmaceutics in the development of a clinical nanoparticle formulation of MK-0869: a Beagle dog model predicts improved bioavailability and diminished food effect on absorption in human. Int J Pharm. 2004;285:135–46.
Singh A, Worku ZA, Van den Mooter G. Oral formulation strategies to improve solubility of poorly water-soluble drugs. Expert Opin Drug Deliv. 2011;8:1361–78.
Kamboj S, Sharma R, Singh K, Rana V. Aprepitant loaded solid preconcentrated microemulsion for enhanced bioavailability: a comparison with micronized aprepitant. Eur J Pharm Sci. 2015;78:90–102.
Kamboj S, Rana V. Formulation optimization of aprepitant microemulsion-loaded silicated corn fiber gum particles for enhanced bioavailability. Drug Dev Ind Pharm. 2016;42:1267–82.
Liu J, Zou M, Piao H, Liu Y, Tang B, Gao Y, et al. Characterization and pharmacokinetic study of aprepitant solid dispersions with soluplus. Molecules. 2015;20:11345–56.
Dhillon R, Ojha R, Bedi N. Preparation, characterization and optimization of poloxamer solid dispersions of a poorly water soluble drug aprepitant. Br J Pharm Res. 2014;4:2436–54.
Rao BC, Vidyadhara S, Sasidhar RLC, Chowdary YA. Dissolution enhancement of poorly soluble drug aprepitant by hot melt extrusion method using hydrophilic polymer: a solid dispersion technique. Res J Pharm Biol Chem Sci. 2014;5:1469–85.
Penumetcha SS, Gutta LN, Dhanala H, Yamili S, Challa S, Rudraraju S, et al. Hot melt extruded Aprepitant-Soluplus solid dispersion: preformulation considerations, stability and in vitro study. Drug Dev Ind Pharm. 2016;42:1609–20.
Sharma R, Kamboj S, Singh G, Rana V. Development of aprepitant loaded orally disintegrating films for enhanced pharmacokinetic performance. Eur J Pharm Sci. 2016;84:55–69.
Ridhurkar DN, Ansari KA, Kumar D, Kaul NS, Krishnamurthy T, Dhawan S, et al. Inclusion complex of aprepitant with cyclodextrin: evaluation of physico-chemical and pharmacokinetic properties. Drug Dev Ind Pharm. 2013;39:1783–92.
Angi R, Solymosi T, Ötvös Z, Ordasi B, Glavinas H, Filipcsei G, et al. Novel continuous flow technology for the development of a nanostructured aprepitant formulation with improved pharmacokinetic properties. Eur J Pharm Biopharm. 2014;86:361–8.
Karavas E, Koutris E, Samara V, Koutri I, Kalaskani A, Kiziridi C, Abatzis M, Bikiaris D, Invetors, Pharmathen S.A., assignee. Pharmaceutical composition comprising aprepitant and method for the preparation thereof. Geneva: World Intellectual Property Organization; 2016.
Klein S. In vitro lipolysis assay as a prognostic tool for the development of lipid based drug delivery systems (Dissertation). der Martin-Luther-Universität Halle-Wittenberg, Datum der öffentlichen Verteidigung: 30.01.2013.
Aprepitant scientific discussion, EMEA. 2004. Available at: https://www.ema.europa.eu/docs/en_GB/document_library/EPAR_-_Scientific_Discussion/human/000527/WC500026534.pdf. Assessed 20 Feb 2017.
Spireas S, Bolton S.M. Liquisolid systems and methods of preparing same, US Patent 5968. 1999. p. 550.
Azharshekoufeh BL, Shokri J, Adibkia K, Javadzadeh Y. Liquisolid technology: what it can do for NSAIDs delivery? Colloids Surf B Biointerfaces. 2015;136:185–91.
Hentzschel CM, Sakmann A, Leopold CS. Suitability of various excipients as carrier and coating materials for liquisolid compacts. Drug Dev Ind Pharm. 2011;37:1200–7.
Singh SK, Srinivasan KK, Gowthamarajan K, Prakash D, Gaikwad NB, Singare DS. Influence of formulation parameters on dissolution rate enhancement of glyburide using liquisolid technique. Drug Dev Ind Pharm. 2012;38:961–70.
El-Hammadi M, Awad N. Investigating the use of liquisolid compacts technique to minimize the influence of pH variations on loratadine release. AAPS PharmSciTech. 2012;13(1):53–8.
Lu M, Xing H, Yang T, Yu J, Yang Z, Sun Y, et al. Dissolution enhancement of tadalafil by liquisolid technique. Pharm Dev Technol. 2017;22:77–89.
Elkordy AA, Tan XN, Essa EA. Spironolactone release from liquisolid formulations prepared with Capryol™90, Solutol® HS-15 and Kollicoat®SR 30D as non-volatile liquid vehicles. Eur J Pharm Biopharm. 2013;83:203–23.
Syed IA, Pavani E. The liquisolid technique: based drug delivery system. Int J Pharm Sci Drug Res. 2012;4:88–96.
Vraníková B, Pavloková S, Gajdziok J. Experimental design for determination of effects of superdisintegrant combinations on liquisolid system properties. J Pharm Sci. 2017;106:817–25.
Tiong N, Elkordy AA. Effects of liquisolid formulations on dissolution of naproxen. Eur J Pharm Biopharm. 2009;73:373–84.
Javadzadeh Y, Shariati H, Movahhed-Danesh E, Nokhodchi A. Effect of some commercial grades of microcrystalline cellulose on flowability, compressibility, and dissolution profile of piroxicam liquisolid compacts. Drug Dev Ind Pharm. 2009;35:243–51.
Elkadi S, Elsamaligy S, Al-Suwayeh S, Mahmoud H. The Development of self-nanoemulsifying liquisolid tablets to improve the dissolution of simvastatin. AAPS PharmSciTech. 2017; https://doi.org/10.1208/s12249-017-0743-z.
Kennard R, Stone L. Computer aided design of experiments. Technometrics. 1969;11:137–48.
Koza JR. Genetic programming as means for programming computers by natural selection. Stat Comput. 1994;4:87–112.
Barmpalexis P, Kachrimanis K, Georgarakis E. Solid dispersions in the development of a nimodipine floating tablet formulation and optimization by artificial neural networks and genetic programming. Eur J Pharm Biopharm. 2011;77:122–31.
EPA, United States Environmental Protection Agency. 2014: 2-Pyrrolidone. Available at http://wwwepagov/oppt/chemrtk/hpvis/hazchar/16455SN1942-pyrrolidonePOSTpdf. Assessed 10 Mar 2017.
Raghavan SL, Trividic A, Davis AF, Hadgraft J. Crystallization of hydrocortisone acetate: influence of polymers. Int J Pharm. 2001;212:213–21.
Baird JA, Van Eardenbrugh B, Taylor LS. A calcification system to assess the crystallization tendency of organic molecules from undercooled melts. J Pharm Sci. 2010;99:3787–806.
Helmy R, Zhou GX, Chen YW, Crocker L, Wang T, Wenslow RM Jr, et al. Characterization and quantitation of aprepitant drug substance polymorphs by attenuated total reflectance fourier transform infrared spectroscopy. Anal Chem. 2003;75(3):605–11.
Matsaridou I, Barmpalexis P, Salis A, Nikolakakis I. The influence of surfactant HLB and oil/surfactant ratio on the formation and properties of self-emulsifying pellets and microemulsion reconstitution. AAPS PharmSciTech. 2012;13:1319–30.
Kabanov AV, Batrakova EV, Alakhov VY. Pluronic block copolymers as novel polymer therapeutics for drug and gene delivery. J Control Release. 2002;82:189–212.
Searson DP. GPTIPS 2: an open-source software platform for symbolic data mining. Chapter 22. In: Gandomi AH, et al., editors. Handbook of Genetic Programming Applications. New York: Springer; 2015.
Acknowledgements
The authors thank Prof. Christos Kontoyiannis of the School of Pharmacy of the University of Patras in Greece for the XRD measurement.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
ESM 1
(DOCX 122 kb)
Rights and permissions
About this article
Cite this article
Barmpalexis, P., Grypioti, A., Eleftheriadis, G.K. et al. Development of a New Aprepitant Liquisolid Formulation with the Aid of Artificial Neural Networks and Genetic Programming. AAPS PharmSciTech 19, 741–752 (2018). https://doi.org/10.1208/s12249-017-0893-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1208/s12249-017-0893-z